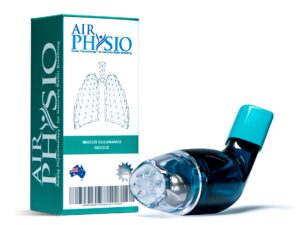


AirPhysio may be able to help by assisting with
✅Clearing the mucus clogging airways
✅Helps Promote Optimal Lung Capacity
✅Helps Promote Optimal Lung Hygiene
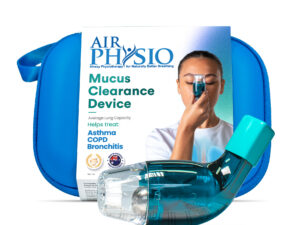
✅Helps treat Respiratory Conditions
✅May Reduce the chance of developing lung infections
✅Recommended by doctors, physical Therapists & Pulmonologists
✅Helps Make Breathing Easier
✅Sold in 106 countries globally


Do you suffer from Dry or Persistent Cough, Breathlessness, Respiratory or Severe Respiratory Conditions, or Shortness of Breath as you Get Older?
THIS PRODUCT MAY NOT BE RIGHT FOR YOU. READ THE WARNINGS BEFORE PURCHASE (Contraindications of Untreated pneumothorax; Tuberculosis; Oesophageal surgery; Right-sided heart failure; Middle ear pathology, such as ruptured tympanic membrane)
FOLLOW THE DIRECTIONS FOR USE
IF SYMPTOMS PERSIST, TALK TO YOUR HEALTH PROFESSIONAL

Gallery
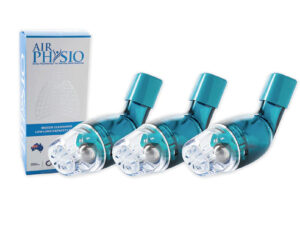
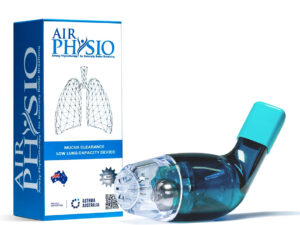
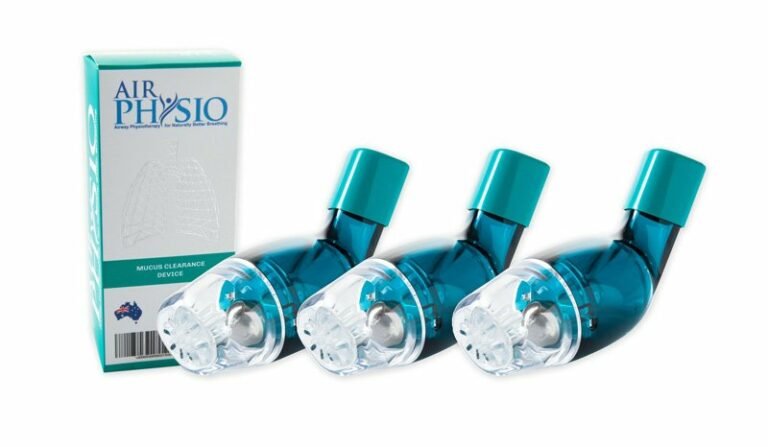
AirPhysio is an Oscillating Positive Expiratory Pressure (OPEP) device that is used for mucus clearance and lung expansion to help in the treatment of respiratory conditions. The use of the AirPhysio device helps to facilitate secretion mobilization and maximize lung volume for cleaner healthier lungs.
© AirPhysio 2022 – All Rights Reserved
| Cookie | Duration | Description |
|---|---|---|
| cookielawinfo-checkbox-analytics | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Analytics". |
| cookielawinfo-checkbox-functional | 11 months | The cookie is set by GDPR cookie consent to record the user consent for the cookies in the category "Functional". |
| cookielawinfo-checkbox-necessary | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookies is used to store the user consent for the cookies in the category "Necessary". |
| cookielawinfo-checkbox-others | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Other. |
| cookielawinfo-checkbox-performance | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Performance". |
| viewed_cookie_policy | 11 months | The cookie is set by the GDPR Cookie Consent plugin and is used to store whether or not user has consented to the use of cookies. It does not store any personal data. |